ABSTRACT
Congenital Verical Talus (CVT) is a rare foot deformity which is most often unrecognised/ misdiagnosed at birth. Inadequate management leads to abnormal gait, shoe wear problems, callosities, pain and functional limitations. Etiology is heterogenous - genetic disorder associated, neuro muscular or idiopathic. Restoration of normal alignment of bones of foot and weight bearing capacity of first ray are primarily aims of treatment. Depending on severity and rigidity of deformities multiple extensive as well as minimal invasive surgical procedures have been described for CVT. In recent times, management has drastically changed from earlier methods of extensive soft-tissue release procedures to the serial manipulation, casting and minimal invasive surgery for Talo navicular joint reduction.
INTRODUCTION
Congenital Vertical Talus, being first described in 1914 by Henke, is one of the causes of congenital rigid flatfoot, inadequate management of which leads to abnormal gait, shoe wear problems, callosities, pain and functional limitations. The rocker-bottom appearance of the medial border of foot, which is classical to this condition, is mostly not apparent at birth, which can lead to the clinician missing the diagnosis, further adding to the problem. The primary pathology in this condition is believed to be the dorsal dislocation of navicular over the talar head, leading to the almost vertical orientation of the talus, a dislocated talonavicular joint, a hindfoot in valgus and equinus and an abducted forefoot. This has been managed classically by extensive surgeries, with soft tissue stripping and release of associated ligamentous contractures and reduction of talonavicular joints.[1][2][3] This is followed by a dreaded course of contractures and suboptimal outcomes for these patients. Dobbs et al,[4] in recent times have presented their management protocol, based on casting and soft tissue stretching, similar to Ponseti philosophy used in clubfoot, followed by minimal invasive talonavicular reduction and tendo-achilles release, with a good, supple, plantigrade feet on short-term follow ups, giving hope of a better management protocol for these patients. This review, gives an overview of current understanding of concepts of CVT and the recent advances in management protocols.
EPIDEMIOLOGY AND ETIOLOGY
EPIDEMIOLOGY
The reported incidence at present is 1 in 10,000, a figure which has continued since the past 20 years,[5] signifying the lack of adequate data and large sample based studies to update the epidemiological data like laterality, ethnicity or other risk factors associated with this disease. It is considered to have an equal incidence in males and females. The indecisive epidemiological data about this condition puts light on the fact that this condition is missed and under-reported. A wider population based and multicentre data would let us know more about the trend, associated risks and when to suspect this condition, which would eventually improve the outcomes.
ETIOLOGY
Half of these cases are considered as isolated or idiopathic in origin, where-as the other half are associated with neuromuscular[6] or genetic disorders[7]. Cause is still not identified, although some evidence indicates, that the deformity is transmitted as an autosomal dominant trait, with incomplete penetrance. Mutations in homeobox transcription factor and cartilage-derived morphogenetic protein-1, are indicated as contributors in some of the familial cases.[8] Although, no single gene can be pointed out and the development of this disorder is essentially heterogenous.
Most commonly associated neurological conditions are arthrogryposis and myelomeningocele, whereas most common genetic conditions found to be associated are aneuploidy of chromosome 13, 15 or 18. Other neurological conditions are disatometamyelia, lipoma of cauda equina, sacral agenesis and neurofibromatosis to name a few.[6] Neurological CVTs are found to be of the more rigid. The imbalance in muscle strength in neurological cases has been postulated to be one of the causes. This is justified by the weak posterior tibialis and the stronger dorsiflexors of ankle, with foot intrinsic muscle contractures or weakness playing a role, as seen in CVT with myelomeningocele. This is further supported by the high number of abnormal muscle biopsies obtained in these patients. A number of syndromes namely DeBarry, Costello, Rasmussen as well as split hand and foot syndromes have been found to be associated with CVT in many cases.Acquired deformities leading to CVT are cerebral palsy, polio, overcorrected clubfoot and spinal muscular atrophy to name a few.
LITERATURE SEARCH
Congenital Vertical Talus is a much talked about topic in the recent times, especially since Dobbs et al. have presented a novel method of minimal invasive management, based on casting principles of Ponseti, which have yielded spectacular results.
A primary PubMed search was done on 1st May 2019 with keywords; (“congenital, Vertical, Talus"[MeSH Terms] OR ("Congenital"[All Fields] AND "Vertical"[All Fields] AND "Talus"[All Fields]).This yielded 2635 results. On adding filters – “Review and 10 years”, the number was bought down to just 155 articles. Of these only 2 articles, had “Congenital Vertical Talus” in their title. On further adding “OR AND ("Paediatric"[MeSH Terms]” narrowed down our search to only 9 review articles. All these articles were primarily reviews about paediatric rigid flatfoot, one of the causes of which is congenital vertical talus.
On using (paediatric rigid flatfoot AND Review [ptyp] AND "last 10 years"[PDat]), gave us only 29 hits, none of which had congenital vertical talus in their title.
PATHOANATOMY
Surgical and autopsy findings have constantly added to understanding of anatomy of soft tissue and bones in a foot with vertical talus.[1][9] The hindfoot is in equinus and valgus due to contracture of Achilles tendon and posterolateral ankle and subtalar joint capsule. Midfoot and forefoot are dorsiflexed and abducted relative to hindfoot secondary to contractures of tibialis anterior, EDL, EHB, peroneus tertius and EHL and dorsal aspect of talonavicular capsule. The navicular is dorsally and laterally dislocated on the head of talus resulting in a hypoplastic and wedge-shaped navicular. Talar head and neck are abnormal in shape and orientation, a flattened head with a medial orientation from the midline. The position of the talus eventually becomes vertical, leading to further stretching of plantar ligaments, namely calcaneonavicular ligament, which leads to the characteristic rocker-bottom foot. Thus, the plantar aspect of the foot is convex, and the dorsal aspect has a deep crease. The equinus position of the calcaneus can further lead to subluxation or dislocation of the calcaneocuboid joint. Within the ankle, only the posterior one third of the talar dome articulates as the calcaneus is plantarflexed and rotated posterolateral. Sustenticulum tali is hypoplastic and provides no support to talar head. The posterior tibial tendon and both the peronei are subluxated anterior to their respective malleoli, which then function as ankle dorsiflexors rather than plantar flexors.[10]
PHYSICAL EXAMINATION AND CLINICAL FEATURES
Paediatric flat foot is one of the most common conditions seen in paediatric orthopaedic practice. The clinician should distinguish between a rigid and non-rigid deformity. The differential diagnosis can include positional calcaneovalgus deformity, posteromedial bowing of tibia, congenital absence of fibula, congenital oblique talus, idiopathic flat feet or CVT.[11]
CVT patients usually present with “Persian slipper foot”,[9] a hindfoot equinus ,hindfoot valgus, forefoot abduction and forefoot dorsiflexion, which are features present in all new born with a vertical talus. The rigidity of these deformities is the key to diagnosis. Also, the talar head is usually palpable at the medially at the sole of the foot. Since this condition is frequently associated with other neuromuscular and genetic conditions, thus a comprehensive examination of the patient should be performed. Any features such as facial dysmorphic features, or spinal dyraphism should alert the clinician to get a genetic or neurological workup. Sacral dimple, in particular should alert the examiner about a central nervous system anomalies.
Documenting the motor function of the extensors and flexors of the toes also plays an important role. Stimulating the dorsal and plantar aspect of foot, in a serial manner, leads to dorsiflexion or plantarflexion response of the toes, This response is graded separately for the greater toe and for the other four toes and rated as absent, slight or definitive. An absent or slight response is indicative of a more rigid CVT. These responses may also be indicative of a neurological or muscular anomaly.[12]
Clinically, the plantar surface is convex with a prominent talar head, the dorsal surface presents with deep creases and on palpation a gap can be felt where the normal talonavicular joint would have articulated. If this gap reduces with plantarflexion, then the deformity can be considered to be flexible. This predicts responsiveness to treatment.
CVT does not delay weight bearing and these patients have a peg-leg gait ( an awkward gait with limited forefoot push-off)[9] with callus under a prominent talar head. The heel does not touch the ground; rather weight bearing occurs only in a half-dollar sized area. With time, shoe wear becomes difficult and painful callosities develop, making ambulation a painstaking job.[13][14]
RADIOGRAPHIC EVALUATION
Radiographic evaluation of paediatric foot is difficult due to the non-ossified nature of the midfoot bones in new borne. Hindfoot and metatarsals are ossified at birth, with midfoot bones appearing subsequently. Cuboid ossifies during the first month and cuneiform and navicular during second and third year respectively. An AP view and three lateral views in maximal dorsiflexion, maximal plantarflexion and neutral should be done. The plantarflexion lateral view is important to assess the rigidity of the talonavicular dislocation. The assessment should primarily focus on relationship between the ossified centres rather than the midfoot bones, which can misguide the clinician.[15][16]
Useful angles on the lateral view include the talocalcaneal angle, tibiocalcaneal angle and the talar-first metatarsal axis angle. On a neutral view, the long axis of talus is vertical in relation to first metatarsal; calcanuem is in significant equinus as seen with the high tibiocalcaneal angle. The forced dorsiflexion and plantarflexion views are important to help assess the rigidity of the deformity and thus differentiate CVT from more flexible deformities like oblique talus or calcaneovalgus foot. In a case of CVT, a lateral view in plantarflexion demonstrates persistent vertical orientation of talus and a view in dorsiflexion demonstrates persistent rigid hindfoot equinus. On the lateral view in plantarflexion, the talar-first metatarsal axis angle can be used to distinguish vertical and oblique talus, with angles >35degrees considered as diagnostic for CVT. However an angle < 35 degrees cannot rule out CVT. Next step in such cases should be looking for the hindfoot equinus deformity. If rigid, then such feet need treatment in a manner similar to CVT feet. An AP talocalcaneal and talar-first metatarsal axis angle can be used as guides, but no angle is pathognomic of this deformity in AP views.[12] Of other imaging modalities, like MRI provide a detailed outline of the cartilage anlage of bones, though use is presently limited to research purposes only.[9]
MANAGEMENT
Restoration of normal alignment of bones of foot and weight bearing capacity of first ray are primarily aims of treatment. Depending on severity and rigidity of deformities multiple extensive as well as minimal invasive surgical procedures have been described for CVT.
Closed treatment and casting, was one of the first treatment strategies used and showed poor results consistently when done as a sole method of management. Jacobsen and Crawford’s performed a literature review in 1983, which emphasized that surgically managed patients had better outcomes as compared to the conservative group.[5] Presently, the most often used protocol is of serial casting which helps to stretch the foot in plantar flexion and inversion while counterpressure is applied to the medial aspect of talus, followed by surgery for reduction of talo-navicular joint.[4] This serial casting and stretching also avoids compression of the navicular head into talus.Any surgical treatment is preferably delayed till the child is 12-18 months old. Earlier surgeries, especially those done before 2 years of age, tend to have a better prognosis.[12] Lamy and Weissman[17] in 1939 recommended excision of talus for rigid flatfoot where as Eyre-Brooke[2] advocated excising the navicular. At present, neither of these techniques is accepted.
Osmond-Clarke (1956),[3] Herndon and Heyman(1963)[16] and Coleman and colleagues[18] (1970) described a staged, two-incision surgical technique. Stage 1 included lengthening of EDB, EHL, Tibialis anterior and capsulotomies of talonavicular and calcanecuboid joints. Second stage included Tendo-achilles lengthening with a posterior capsulotomy of ankle and subtalar joints.
In 1979, Ogata and colleagues[19] recommended a single-stage approach noticing the high complication rate following the staged procedures. In 1987, Seimon came forward with a single stage dorsal approach.[1]Seimon propagated the idea of correcting both the forefoot and hindfoot deformities. In his approach, EHL and Peroneous Tertius were tenotomised and talonavicular joint was opened. This joint was further fixed with a K-wire and a percutaneous TA tenotomy was done. This procedure yielded very good results in their study, leading them to conclude that there was no need of extensive surgery or a two-staged surgery to be done. Stricker et al[20]published their experience with the Seimon’s one-stage method, and found very good results to obtain a plantigrade feet at 41 months despite the presence of ankle and subtalar stiffness and some evidence of residual forefoot abduction on radiographs.
Mazzocca et al[21] in their study, compared the results between Seimon’s one stage surgery and posterior approach for CVT. They found similar radiographic results with both the procedures, but they found that posterior approach had more complications, increased operative time and poorer clinical scores.
Kodros et al[22] described a single-stage approach with Cincinnati incision, an incision from medial cuneiform to lateral malleolus that could be extended to calcaneocuboid joint. They reported good clinical and radiological results, with normalization of AP and lateral talo-calcaneal and talar-first metatarsal angles, but a number of feet in their series needed re-surgeries.
Dobbs et al[4] presented their method of treatment of CVT, via even less surgery as compared to previous guidelines. They combined closed manipulation, K-wire fixation of talonavicular joint and percutaneous heel cord release. They noticed that earlier procedures of extensive surgical release were associated with complications like postoperative stiffness, wound necrosis, AVN of talus, pseudo-arthrosis, under-correction of deformities as well as need for further surgeries.
Casting was done a method similar to Ponseti’s method for clubfoot, with forces applied in opposite direction and medial talar head used as fulcrum for correction. The foot is manipulated into a plantarflexion and inversion position with one hand and the thumb of the other hand is used to push the talar head into a dorsal and lateral position. Calcaneus is not manipulated at this stage. All deformities of CVT are corrected in a sequential manner, except equinus which is corrected last (Reverse Ponseti Technique). After a couple of minutes of stretch, a long leg plaster is applied in a fashion similar to the clubfoot casts, but with foot in equinovarus. Cast application should start as soon as possible and usually takes about 5 to 6 casts for complete stretching of soft tissue and ability to reduce talonavicular joint. The position in the final cast is of extreme equinovarus resembling a clubfoot. This is followed by fixation of a reduced talo-navicular joint. For this a dorsomedial incision is given and inspection of congruent joint reduction is done. If the joint is reduced a retrograde K-wire is passed without opening the capsule. If the joint is not congruently reduced, capsulotomy is done and K-wire is passed after reduction. K wire is buried to avoid backing out. In non-isolated, rigid CVT there is also contracture of other soft tissue structures like tibialis anterior, peroneous brevis or dorsal extensor tendons which are then lengthened. Finally, a percutaneous Tendo Achilles tenotomy is done to correct the residual equinus. The foot is immobilized in cast with forefoot and hindfoot in neutral and changed at 2 weeks to add 10 degrees dorsiflexion. K-wire is removed at 6 weeks postoperatively followed by a shoe-bar-brace system worn fulltime for 2 months, followed by night time wearing for 2 years, to prevent relapse. It is imperative to ensure that there is no dorsiflexion in the boots used with the bar. The parents are also taught frequent stretching of the feet, especially at diaper change to reduce the chances of relapse. Once the child starts walking he is given a day-time brace and an Ankle-Foot Orthosis to walk. Since the year 2006, multiple studies have been published which validate this method of management as uniformly producing good results.[10][23][24][25]
SUMMARY
CVT is an uncommon foot deformity and a cause for rigid flat or convex (rocker-bottom) feet in children. A non-suspecting clinician can easily miss the diagnosis in view of looking only for clubfoot in new born and thus lead to a prolonged and tedious path of management. A thorough clinical examination, suspicion and radiology can allow the orthopedician to diagnose as well as start management as soon as possible thus improving outcomes. Management has drastically changed from earlier methods of extensive soft-tissue release procedures to the present favourite of manipulation, casting and minimal invasive surgery. This method has yet produced uniformly good results, although long term results are still to be looked for.
BIBLIOGRAPHY
1.Seimon LP. Surgical correction of congenital vertical talus under the age of 2 years. J Pediatr Orthop. 7(4):405-11.
2.Eyre-Brook AL. Congenital vertical talus. J Bone Joint Surg Br. 1967 Nov;49(4):618–27.
3.OSMOND-CLARKE H. Congenital vertical talus. J Bone Joint Surg Br. 1956 Feb;38-B(1):334-41.
4.Dobbs MB, Purcell DB, Nunley R, Morcuende JA. Early Results of a New Method of Treatment for Idiopathic Congenital Vertical Talus. J Bone Jt Surg. 2006 Jun;88(6):1192-200.
5.Jacobsen ST, Crawford AH. Congenital vertical talus. J Pediatr Orthop. 1983 Jul;3(3):306-10.
6.Sharrard WJ, Grosfield I. The management of deformity and paralysis of the foot in myelomeningocele. J Bone Joint Surg Br. 1968 Aug;50(3):456-65.
7.Merrill LJ, Gurnett CA, Connolly AM, Pestronk A, Dobbs MB. Skeletal Muscle Abnormalities and Genetic Factors Related to Vertical Talus. Clin Orthop Relat Res. 2011 Apr 20;469(4):1167-74.
8.Dobbs MB, Gurnett CA, Pierce B, Exner GU, Robarge J, Morcuende JA, et al. HOXD10 M319K mutation in a family with isolated congenital vertical talus. J Orthop Res. 2006 Mar;24(3):448-53.
9.Drennan JC. Congenital vertical talus. Instr Course Lect. 1996;45:315-22.
10.Alaee F, Boehm S, Dobbs MB. A new approach to the treatment of congenital vertical talus. J Child Orthop. 2007 Sep;1(3):165-74.
11.Sankar WN, Weiss J, Skaggs DL. Orthopaedic conditions in the newborn. J Am Acad Orthop Surg. 2009 Feb;17(2):112-22.
12.Miller M, Dobbs MB. Congenital Vertical Talus. J Am Acad Orthop Surg. 2015 Oct;23(10):604-11.
13. HARRIS RI, BEATH T. Hypermobile flat-foot with short tendo achillis. J Bone Joint Surg Am. 1948 Jan;30A(1):116-40.
14.Brand RA. 50 years ago in CORR: Congenital vertical talus. Tom Outland MD and Henry H. Sherk MD CORR 1960;16:214-218. Clin Orthop Relat Res. 2010 Oct;468(10):2822-4.
15.Vanderwilde R, Staheli LT, Chew DE, Malagon V. Measurements on radiographs of the foot in normal infants and children. J Bone Joint Surg Am. 1988 Mar;70(3):407-15.
16.Mckie J, Radomisli T. Congenital Vertical Talus: A Review. Clin Podiatr Med Surg. 2010 Jan;27(1):145-56.
17.D Duncan RD, Ed F, Fixsen JA. THE JOURNAL OF BONE AND JOINT SURGERY Congenital convex pes valgus. J Bone Joint Surg [Br]. 1999.
18.Coleman SS, Stelling FH, Jarrett J. Pathomechanics and treatment of congenital vertical talus. Clin Orthop Relat Res. 70:62-72.
19.Ogata K, Schoenecker PL, Sheridan J. Congenital vertical talus and its familial occurrence: an analysis of 36 patients. Clin Orthop Relat Res. (139):128-32.
20.Stricker SJ, Rosen E. Early One-Stage Reconstruction of Congenital Vertical Talus. Foot Ankle Int. 1997 Sep 28;18(9):535-43.
21.Mazzocca AD, Thomson JD, Deluca PA, Romness MJ. Comparison of the posterior approach versus the dorsal approach in the treatment of congenital vertical talus. J Pediatr Orthop. 21(2):212-7.
22.Kodros SA, Dias LS. Single-stage surgical correction of congenital vertical talus. J Pediatr Orthop. 19(1):42-8.
23.Chalayon O, Adams A, Dobbs MB. Minimally Invasive Approach for the Treatment of Non-Isolated Congenital Vertical Talus. J Bone Jt Surgery-American Vol. 2012 Jun 6;94(11):e73-7.
24.Rodriguez N, Choung DJ, Dobbs MB. Rigid Pediatric Pes Planovalgus: Conservative and Surgical Treatment Options. Clin Podiatr Med Surg. 2010 Jan;27(1):79-92.
25.Eberhardt O, Fernandez F, Wirth T. Die Behandlung des Talus verticalis mit der Methode nach Dobbs. Z Orthop Unfall. 2011 Apr 5;149(02):219-24.
AUTHORS CONTRIBUTION
Dr. Karthick S. R
Concept, Acquisition of data, Revision of Article
Dr. Pulak Vatsya
Drafting of Article, Concept and Design
Dr. Nirmal Raj Gopinathan
Critical Revision of Article
Dr. Prashant Sharma
Concept and Acquisition of data.
Illustrations
Illustration 1: Clinical picture of child showing rocker- bottom foot.
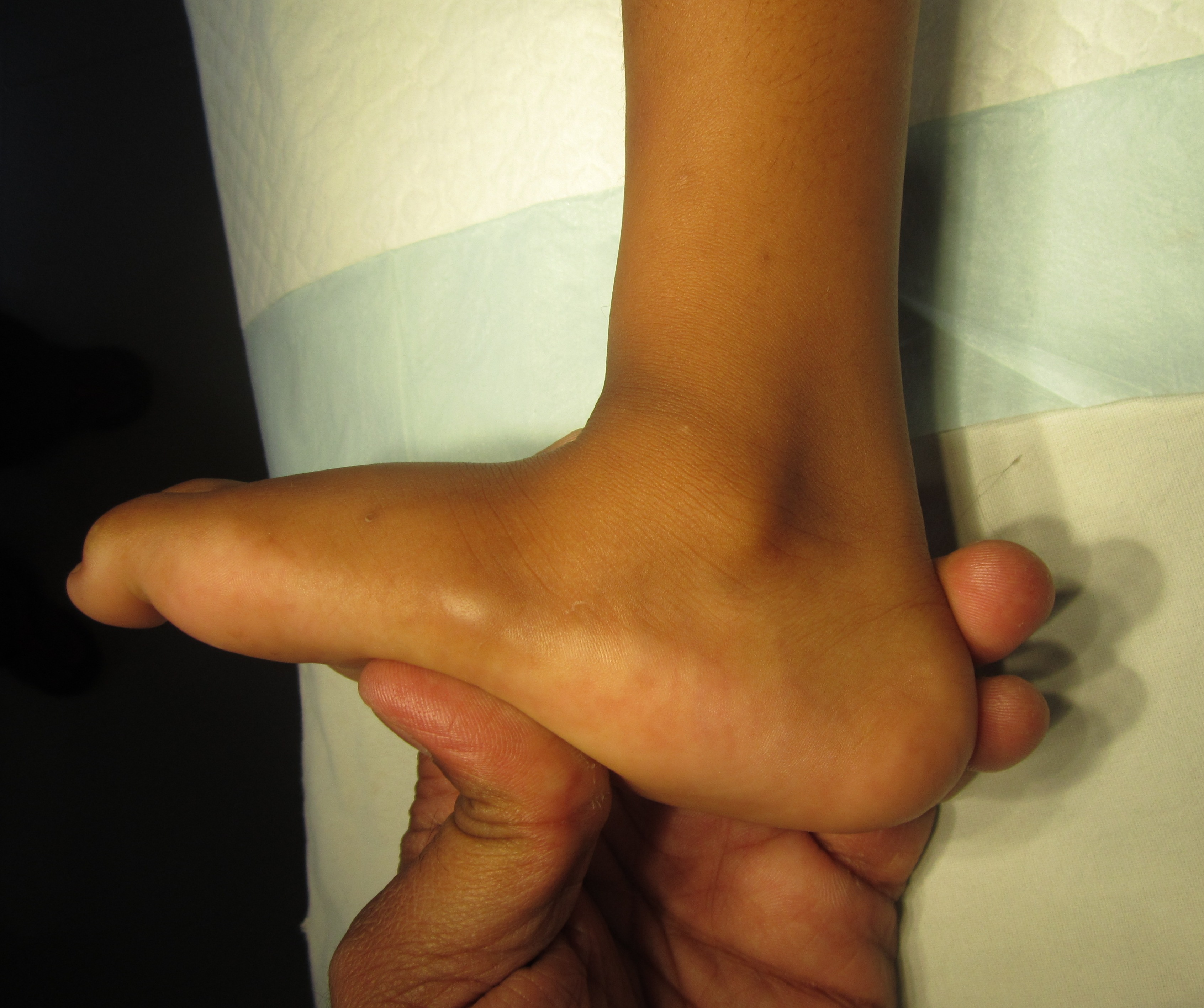
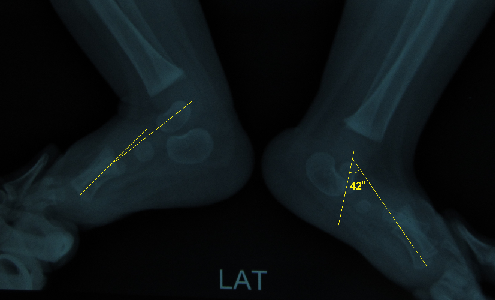
Illustration 2: Lateral view with forced plantar flexion showing vertical talus (talar- first metatarsal axis angle > 35?) on left foot.
Illusration 3: AP radiograph of foot showing Angle X – Talar first metatarsal axis angle and Angle Y – Talo calcaneal angle.
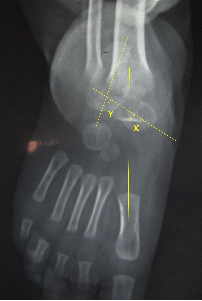
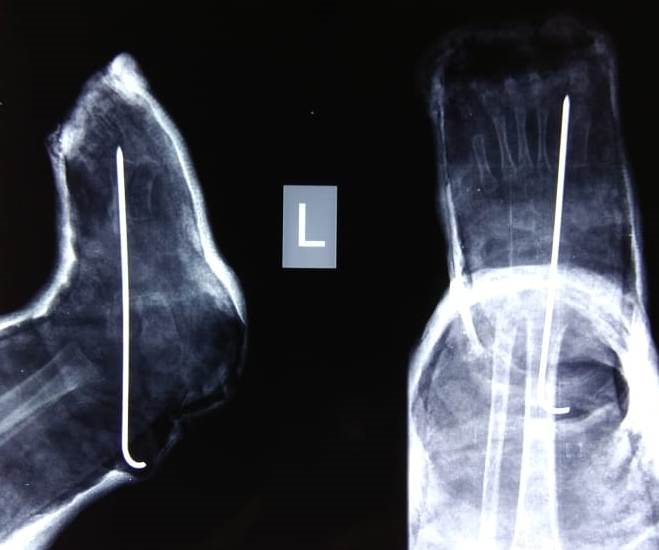
Illustration 4: Post op Xray showing Talo navicular joint reduced and fixed with a K wire.
Source(s) of Funding
No source of funding
Competing Interests
Conflict of interest : Nil
 All site content, except where otherwise noted, is licensed under a
Creative Commons Attribution License
All site content, except where otherwise noted, is licensed under a
Creative Commons Attribution License